Ketamine Therapy for Depression: A New Frontier in Mental Health Treatment

Depression is frequently discussed in low tones. Many people carry it discreetly while still meeting the demands of their jobs, families, and daily lives. Despite this quiet, one of our time’s most serious public health concerns remains. According to the World Health Organization, depression affects hundreds of millions of people globally and is still a primary cause of disability.
For many people, treatment with psychotherapy and antidepressants delivers significant alleviation. Despite obtaining appropriate care, a large percentage of people continue to struggle. In recent years, physicians and researchers have begun investigating new therapies that may benefit patients who have not received relief from traditional approaches. Among these developing alternatives, ketamine therapy has received a lot of interest in psychiatric care.
Understanding What is Depression
To grasp the significance of developing medicines, ask a simple question: What is depression?
Depression is a medical disorder that affects one’s mood, thought patterns, energy levels, and physical health. It is more than just a period of grief or a bad week. Clinical depression is characterised by long-term changes in a person’s feelings, thoughts, and functioning.
Depression is sometimes referred to in medical terms as major depressive disorder, a condition marked by a persistent poor mood or a loss of interest in previously significant activities. These alterations can have an impact on sleep, hunger, attention, and enjoyment.
Psychiatric researchers consider depression to be a complicated illness involving several biological and psychological systems. Brain chemistry, genetics, stress exposure, and life events all have an impact. Neurotransmitters, including serotonin, dopamine, and glutamate, affect how brain cells communicate. When these systems are out of balance, emotional control and motivation might suffer.
Depression can strike at any stage of life. Some people have only one episode, while others have repeated cycles that last for years. Early diagnosis of the disease might assist patients in seeking appropriate assistance and treatment.
Recognising the Symptoms of Depression
The symptoms of depression often develop gradually. At first, they may appear as subtle shifts in mood or energy. Over time, they can begin to affect daily functioning.
Common depression symptoms include:
- Persistent sadness or low mood
- Loss of interest in activities that were once enjoyable
- Fatigue or reduced energy
- Changes in sleep patterns, including insomnia or excessive sleeping
- Changes in appetite or body weight
- Difficulty concentrating or making decisions
- Feelings of guilt, hopelessness, or worthlessness
- Slower movement or agitation
- Social withdrawal
- Thoughts of self-harm or suicide in severe cases
These signs of depression vary from person to person. Some individuals experience primarily emotional symptoms, while others notice physical changes such as exhaustion, headaches, or digestive discomfort.
It is also possible for depression to exist alongside anxiety, trauma-related conditions, or chronic stress. Many people continue to function professionally while experiencing internal emotional numbness or detachment. This presentation is sometimes described informally as high-functioning depression.
Recognising these patterns early can allow individuals to access appropriate care before symptoms deepen.

Conventional Treatments for Depression
Modern psychiatry offers several evidence-based treatments for depression. These typically include:
Psychotherapy
Therapies such as cognitive behavioural therapy and trauma-informed counselling help individuals understand thought patterns and develop healthier coping strategies.
Antidepressant medication
Medications such as selective serotonin reuptake inhibitors aim to stabilise neurotransmitter systems that influence mood regulation.
Lifestyle and behavioural interventions
Exercise, sleep regulation, social connection, and stress management all play supportive roles in recovery.
For many individuals, these treatments offer meaningful improvement. However, approximately one-third of people with depression experience what clinicians describe as treatment-resistant depression, where symptoms persist despite multiple treatment attempts.
This challenge has prompted researchers to explore new pharmacological approaches that work through different biological pathways.
The Emergence of Ketamine Therapy
Ketamine has been used in medicine for decades as an anaesthetic. It was first developed in the 1960s and later approved for surgical use because of its reliable safety profile in controlled clinical environments.
In the early 2000s, psychiatric researchers began observing something unexpected. Patients receiving low doses of ketamine during clinical studies reported rapid improvements in depressive symptoms. These findings sparked a wave of research into ketamine therapy for depression.
Today, ketamine is being studied and used in specialised clinical settings for individuals who have not responded fully to conventional treatments. It is important to emphasise that therapeutic ketamine is administered under strict medical supervision with carefully calibrated protocols.
The goal is not sedation but the creation of a temporary neurological state that allows the brain to reorganise emotional patterns.
How Ketamine Affects the Brain
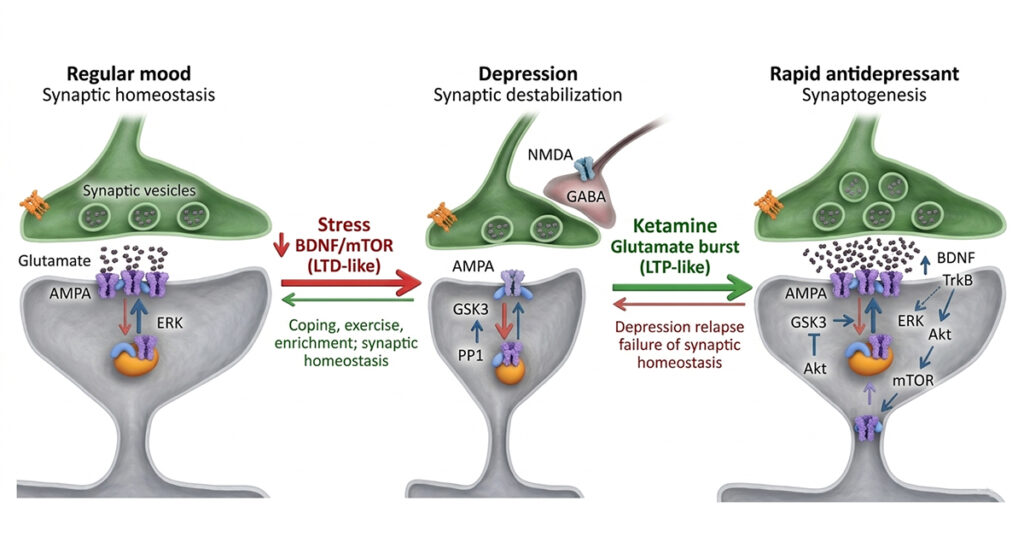
Traditional antidepressants typically influence the serotonin and norepinephrine systems. Ketamine works via a distinct method that involves the brain’s glutamate signalling network.
Glutamate is the most common excitatory neurotransmitter in the human brain. It is crucial for learning, memory, and brain transmission.
Research shows that ketamine temporarily blocks NMDA receptors in this system. This action initiates a series of biological events that enhance glutamate release and promote the development of new synaptic connections.
Simply put, ketamine may aid the brain in the formation of new neural communication pathways. Scientists refer to this ability as neuroplasticity.
According to studies by institutes such as the National Institute of Mental Health, increased neuroplasticity may help individuals absorb emotions and experiences in novel ways, particularly when therapy is incorporated into treatment.
These biochemical changes may explain why some people experience changes in mood, perspective and emotional flexibility after receiving carefully monitored treatment.
Understanding Ketamine Effects in Clinical Care
The effects of ketamine during therapeutic sessions differ from person to person. In a regulated clinical setting, the medicine is usually given in modest dosages by intravenous infusion, oral formulations, or other medically supervised delivery techniques.
These doses are substantially lower than those used for anaesthesia.
During treatment, some people report experiences like these:
- A sense of alienation from normal mental patterns
- Enhanced introspection.
- Visual or sensory alterations
- Emotional insights
These effects are transient and typically disappear within a few hours. Medical staff monitors patients throughout the session to ensure their safety and comfort.
Researchers believe that psychological experience, paired with biological changes in neuroplasticity, may open up a window for more effective therapeutic reflection.
Ketamine Dose and Treatment Protocols
Determining the appropriate ketamine dose requires careful medical evaluation. Factors such as medical history, current medications, and mental health profile are all considered before treatment begins.
Clinical protocols generally involve a series of low-dose sessions administered over several weeks. Each session is supervised by trained medical professionals who monitor vital signs and patient well-being.
Because ketamine influences brain chemistry and perception, responsible clinics follow strict screening procedures. This ensures that the treatment is suitable for the individual and that risks are minimised.
The field of ketamine assisted therapy continues to evolve as new clinical trials expand our understanding of optimal dosing strategies and long-term outcomes.
Ketamine Therapy in a Therapeutic Setting
While the pharmacological effects of ketamine are important, many clinicians emphasise the role of the surrounding therapeutic environment.
The treatment setting often includes psychological support, integration sessions, or reflective practices that help individuals process insights that may arise during treatment.
This integrative approach acknowledges that depression involves emotional patterns, life experiences, and neurological processes. Addressing all of these elements can help create a more supportive pathway toward recovery.
Our Approach at Soma Wellness Clinic
At Soma Wellness Clinic, we approach ketamine therapy with careful clinical oversight and a deep respect for the complexity of mental health.
Our protocol uses low-dose ketamine therapy in a structured medical setting designed to support emotional reset. Each treatment is conducted under the supervision of qualified physicians and follows applicable medical and regulatory standards.
We see ketamine as a therapeutic tool rather than a standalone solution. When appropriate, it is paired with psychotherapy, journaling, breathwork, or reflective practices. This integrated approach helps individuals explore the insights that may arise during treatment and translate them into lasting emotional change.
Our programme is designed for individuals who may be facing:
- Anxiety or trauma-related challenges
- High-functioning depression or emotional numbness
- Limited response to traditional talk therapy or antidepressant medication
Within a guided timeframe, carefully measured microdoses are administered in a safe clinical environment. The intention is to support neuroplasticity and allow the brain to develop healthier adaptive pathways.
Many individuals describe a renewed ability to access feelings of connection, clarity, and emotional flexibility after treatment. Progress can sometimes emerge within weeks, although each person’s experience remains unique.
Our role is to provide a supportive and medically responsible environment in which individuals can explore this emerging therapeutic pathway.
A Developing Field in Mental Health Care
Ketamine therapy has introduced a promising direction in the treatment of depression. By acting on different neural pathways and supporting neuroplasticity, it has expanded how clinicians understand and approach difficult to treat depression.
At the same time, this therapy requires careful screening, precise dosing, and medical supervision. Responsible clinical settings combine ketamine treatment with psychological support to ensure safety and meaningful outcomes. For individuals who have struggled with persistent depression, these advances represent a new possibility in mental health care.
At Soma Wellness Clinic, we offer medically supervised ketamine therapy designed to support emotional healing in a safe and structured environment. If you would like to explore whether this approach may be suitable for you, our team is here to help.
References
- World Health Organization
https://www.who.int/news-room/fact-sheets/detail/depression
- National Institute of Mental Health
https://www.nimh.nih.gov/health/topics/depression
- Cleveland Clinic Ketamine Therapy
https://my.clevelandclinic.org/health/treatments/ketamine-therapy
- National Institutes of Health – Mechanisms of Ketamine in Depression
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7225830
- Depression Overview
https://en.wikipedia.org/wiki/Major_depressive_disorder
- Mental Health Conditions: Depression and Anxiety
https://www.cdc.gov/tobacco/campaign/tips/diseases/depression-anxiety.html
- Ketamine Medical Overview
https://en.wikipedia.org/wiki/Ketamine
- Harvard Health Publishing: Ketamine for treatment-resistant depression: When and where is it safe?
- University of Utha: FAST FACTS ABOUT KETAMINE FOR DEPRESSION
https://healthcare.utah.edu/healthfeed/2026/01/fast-facts-about-ketamine-depression
- Yale Medicine: Ketamine for Depression: How It Works
https://www.yalemedicine.org/news/ketamine-for-depression
- Mediclinic: Ketamine infusions: a breakthrough treatment for some patients with depression
FAQs
1. How does ketamine therapy help with depression?
Ketamine works differently than other antidepressants. It affects the brain’s glutamate system and may aid in the formation of new synaptic connections. This method can help some people improve their emotional flexibility and minimise their depression symptoms.
2. Who can consider ketamine therapy for depression?
Ketamine therapy is often explored by people who have not seen enough improvement with antidepressants or talk therapy. A doctor will always assess whether this treatment is suitable before starting.
3. What happens during a ketamine therapy session?
In a clinical setting, a small and carefully monitored ketamine dose is given under medical supervision. Some people feel relaxed or reflective during the session. The ketamine effects usually wear off within a few hours.
4. Is ketamine therapy safe?
When done in a medical clinic with trained professionals, ketamine therapy for depression is carefully monitored and controlled. Doctors screen patients, manage the dose, and observe the entire session to ensure safety.
Leave a Reply